|
These infants exhibit poor feeding, lethargy, tachypnea, costal-sternal retractions, grunting, nasal flaring, tachycardia, or hepatomegaly. Unscreened infants present within the first two weeks for evaluation of a heart murmur or with symptoms of CHF resulting from increased blood flow to the lungs. In the first few days after birth, the critical congenital heart defect (CCHD) screen in these patients show pre-and post-ductal oxygen saturation less than 95% with mild or unnoticeable cyanosis. The clinical picture is driven by the PBF as well as the presence of valvular abnormalities and aortic arch obstruction. The mixing of pulmonary and systemic blood before departure from the heart combined with the degree of pulmonary blood flow (PBF) and pulmonary vascular resistance (PVR) drives the pathophysiology and the clinical picture. This results in worsening cyanosis or right-to-left shunt (Eisenmenger syndrome). As the pulmonary vascular disease worsens, PVR increases. 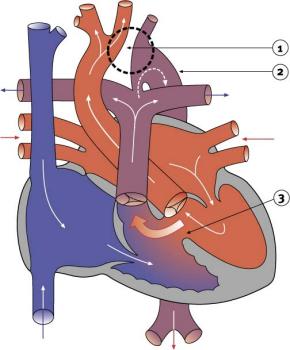
If left untreated, pulmonary over-circulation may eventually lead to severe irreversible pulmonary vascular disease and death. As the PVR drops and PBF increases, pulmonary over-circulation causes congestive heart failure (CHF). Throughout fetal development and the first week of life, PVR is relatively high, resulting in greater shunting of mixed oxygenated and deoxygenated blood into the systemic circuit causing mild cyanosis. Collett and Edwards based their system solely on the origins of the pulmonary vascular system, while Van Praagh also took into account aortic abnormalities. Depending on the origins of the pulmonary arteries, Collett and Edwards (CE) and Van Praagh each classified various forms of TA. These abnormalities include right-sided, interrupted, or hypoplastic aortic arches, abnormal origins of the coronary arteries, pulmonary artery stenosis, and patent ductus arteriosus. The presence of a single arterial trunk can be associated with several cardiac, aortic, and pulmonary abnormalities. 
The common semilunar valve may have 1 to 4 cusps with tricuspid most frequently seen. The VSD allows oxygenated and deoxygenated blood to mix before it is ejected through a common truncal valve to a single great artery, subsequently supplying the coronary, pulmonary and systemic circulations. Pulmonary venous blood from the lungs normally flows through the pulmonary veins into the left atrium and to the left ventricle. In patients with TA, systemic venous blood normally returns to the right atrium and flows into the right ventricle. To understand the pathophysiology of TA, it is first important to understand the path of blood flow and anatomy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
